Cervical Mucus: Your Body’s Fertility Guide Explained
Cervical mucus is more than just a natural fluid; it plays a vital role in women’s reproductive health and fertility. Its appearance, texture, and volume change throughout the menstrual cycle, providing essential clues about ovulation and the best time for conception.
Understanding these changes can help women track their fertility, identify potential health issues, and make informed decisions about reproductive care. This guide explores how cervical mucus is produced, its role in fertility and early pregnancy, factors that affect its quality, and clinical evaluation methods offered at SRM Global Hospitals to support women’s reproductive well-being.
How Cervical Mucus is Produced?
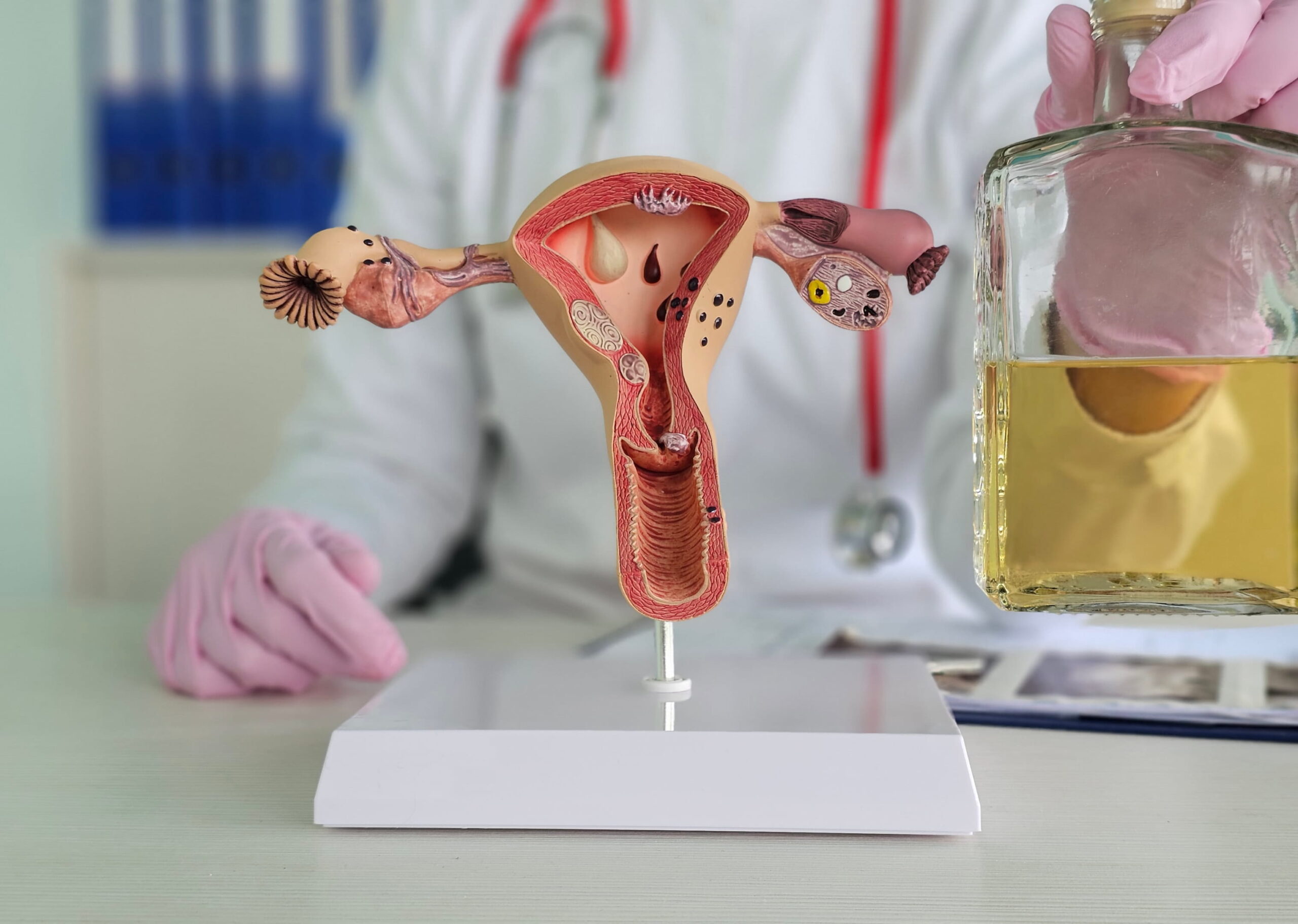
Cervical Mucus Throughout the Menstrual Cycle
Distinct stages of cervical mucus occur throughout a typical 28-day cycle:
- Menstrual Period: Cervical mucus is minimal, and menstrual blood dominates vaginal discharge.
- Early Follicular Phase: Cervical mucus remains sparse, sticky, or dry, with very little cervical mucus present. Fertility remains low.
- Pre-Ovulation / Fertile Phase: Egg white cervical mucus appears 1–2 days before ovulation. Fertile cervical mucus is clear, stretchy, and slippery, resembling raw egg whites. Its presence supports sperm survival for several days and increases the chance of getting pregnant.
- Post-Ovulation / Luteal Phase: Rising progesterone levels cause cervical mucus to become thicker, creamy, or opaque. This cervical mucus consistency acts as a natural barrier against sperm and pathogens.
Fluctuating hormone levels primarily drive cervical mucus changes throughout the menstrual cycle. Tracking these changes helps women predict ovulation, identify the most fertile days, and monitor reproductive health.
Cervical Mucus and Fertility
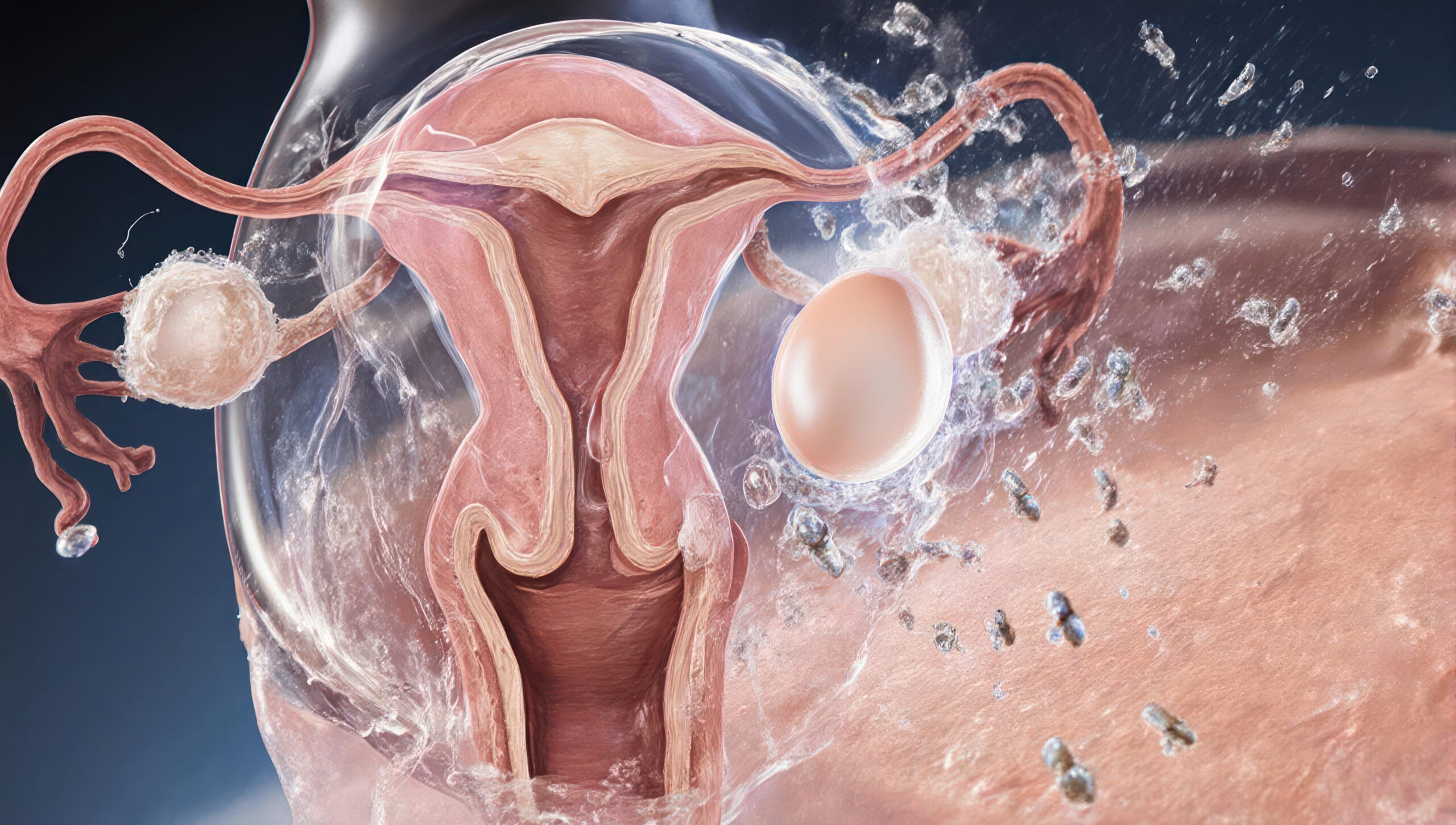
The primary function of cervical mucus is to facilitate conception by helping sperm move through the cervix. Slippery cervical mucus during the fertile time allows intercourse to result in higher chances of fertilisation. Women can monitor cervical mucus by checking consistency and appearance daily, using a clean finger or toilet paper. Fertility treatments may also include cervical mucus monitoring to enhance the probability of conception.
Cervical mucus acts as a natural fertility indicator. Fertile cervical mucus typically appears as transparent, stretchy fluid, while non-fertile mucus is thick and sticky. Tracking cervical mucus changes enables women to identify peak fertility, predict ovulation, and time intercourse effectively.
Cervical Mucus in Early Pregnancy

Abnormal Cervical Mucus
Changes in cervical mucus may indicate underlying health issues:
- Infections: Yellow, green, or foul-smelling discharge, along with itching or burning, may indicate bacterial or protozoan infection and require consultation with a healthcare provider.
- Hormonal Irregularities: Persistent thick, white, non-stretchy mucus may suggest conditions such as polycystic ovarian syndrome (PCOS).
- External Factors: Hormonal birth control, certain medications, dietary supplements, smoking, and lifestyle factors can affect cervical mucus consistency and volume.
Factors Affecting Cervical Mucus Quality
- Hydration: Adequate water intake is critical, as mild dehydration can reduce cervical mucus volume by 15–20%.
- Medications and Contraceptives: Hormonal contraception is designed to thicken cervical mucus, reducing fertility, while some antihistamines may inadvertently dry it out.
- Lifestyle and Diet: Poor nutrition or smoking can reduce cervical mucus elasticity and alter pH, making it less supportive for sperm survival.
- Other Factors: Health conditions, stress, and hormonal changes may also affect cervical mucus patterns and quality.
Clinical Evaluation of Cervical Mucus
Professional assessment at SRM Global Hospitals in Chennai provides precise insight into reproductive health. Diagnostic evaluation includes:
- Visual Inspection: Checking for raw egg white appearance to identify fertile cervical mucus.
- Spinnbarkeit Test: Measures stretchability under a microscope; fertile cervical mucus typically stretches beyond 8 centimetres.
- pH Measurement: Ensures cervical fluid supports sperm survival (pH ≥ 7).
- Ultrasound Correlation: Combines physical checks with transvaginal imaging to correlate cervical mucus changes throughout the cycle with follicle growth and ovulation timing.
Management and Clinical Guidance
Treatment strategies focus on restoring optimal cervical mucus production and overall reproductive health:
- Hormonal Therapy: Corrects cycle imbalances, improving fertile cervical mucus.
- Antimicrobial Treatments: Clear infections and restore healthy vaginal discharge.
- Lifestyle and Nutrition: Adequate hydration, essential vitamins, and cessation of smoking enhance cervical mucus quality.